People who cannot eat independently or have difficulty swallowing, chewing, or both can receive liquid nutrition through feeding tubes. It might be challenging to decide whether to need a feeding tube, especially for older people. One day, family carers may have to make this tough decision for an ageing loved one. Therefore, knowing when and why tube feeding is acceptable is critical. In this blog, we’ll learn when is it wrong to use feeding tube in elderly.

Kinds of Feeding Tubes That Elders May Require
There are differences in the lengths of time and uses for different kinds of feeding tubes. The names of each type of feeding tube often represent the sites of the tube’s entry and departure from the body.
Feeding tubes that are inserted non-surgically
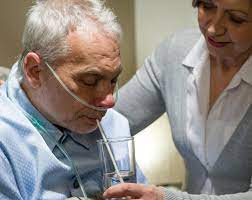
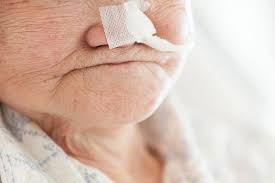
Temporary feeding tubes can be inserted via the nasal or oral routes. The tube can conclude the duodenum, jejunum, or stomach (gastric), depending on where the body needs nutrition, fluids, and/or medication. The nose inserts nasogastric tubes (NG tubes), whereas orogastric tubes (OG tubes) are positioned by the mouth and end up in the stomach.
For short-term tube feedings, non-surgically implanted feeding tubes are usually utilized as a person recovers and their capacity to eat safely improves. If used for over a few weeks, the nose, throat, and oesophagus tissues may become severely irritated and injured.
Feeding tubes inserted surgically
Percutaneous feeding tubes are implanted through a surgical incision known as an ostomy or stoma in the abdominal wall. The more intrusive tubes can be removed if a patient regains the capacity to eat and drink independently. Usually, these tubes are implanted for long-term or permanent usage. Percutaneous tubes, like nasal and oral tubes, can terminate in the small intestine or the stomach (sometimes called a gastrostomy tube or G-tube).
Why Do We Use Feeding Tubes?
For various causes, people of different ages may require a feeding tube either temporarily or permanently. Patients may not be able to eat effectively owing to specific head, neck, and oesophagal cancers, head trauma, traumatic brain injury (TBI), stroke, and neurological diseases, including Parkinson’s disease and dementia. Feeding tubes may also be recommended for those who have become malnourished as a result of their reluctance to eat.
When is it wrong to use feeding tube in elderly?
An elderly patient’s quality of life or care goals are compromised when a feeding tube is used. A decision to refuse tube feeding may be made due to several circumstances, such as advanced dementia, terminal illness, or irreversible conditions when the operation has more drawbacks than positives, such as a shortened life expectancy, increased complications, or a lower quality of life.
In these situations, medical professionals prioritize symptom treatment, comfort-focused care, and respecting the patient’s choices. They may even decide to utilize different types of hydration or nourishment that align with the patient’s desires and general well-being.
The Decision to Place a Feeding Tube
Whatever their form, feeding tubes have a valuable function, especially for those who do not have an incurable disease. Sadly, not every patient who cannot eat or refuses to eat can benefit from tube feeding; thus, each patient’s situation should be evaluated individually. “[Artificial nutrition and hydration] should be evaluated by weighing its benefits and burdens in light of the patient’s clinical circumstances and goals of care,” the American Academy of Hospice and Palliative Medicine said in a position statement.
Also Read : Non Bedside Nursing Jobs : A Comprehensive Guide
This is only one significant end-of-life concern many elderly and family carers face. To ensure that one another’s intentions are honoured and to prevent confusion, families must discuss and document their preferences for end-of-life care as soon as possible.
Living wills and advance directives—such as physician orders for life-sustaining treatment (POLST) forms and do-not-resuscitate (DNR) orders—are essential to document end-of-life care decisions. These documents should specify if, when, and how long a person wishes to be nourished in this way.
Ultimately, it’s not easy to decide whether to use a feeding tube for oneself or as a career for another person. It takes time and effort for medical professionals and families to thoroughly examine the benefits and drawbacks of feeding tubes and alternatives. Still, the work is well worth the investment.

The Pros and Cons of Elderly Feeding Tubes
Pros
- A practical solution for senior citizens suffering from long-term illnesses who are incapable of feeding themselves or need assistance from a carer. A doctor may remove the tube in less than a minute if it is no longer needed.
- Elderly patients with gas, bloating, vomiting, and nausea are frequently treated with feeding tubes; in addition to aiding digestion, a feeding tube’s primary function is to prevent food or liquids from entering the lungs, which can result in aspiration pneumonia.
Cons
- A feeding tube misplacement in the trachea can cause asphyxia, pain, and pneumonia.
- Feeding tubes have been associated with stomach, oesophageal, and nasal airway erosions and abrasions, some of which may result in bleeding. If a feeding tube becomes obstructed, dislodged, or damaged, it can cause significant complications like ulcers and throat, sinuses, and stomach infections. Patients may want to rip the tube out if they are in discomfort. Thus, restraining is necessary.
Considerations for Feeding Tube Care
Many factors must be taken into account while providing care for people who have feeding tubes. To avoid issues like infection or dislodgement, it is essential to evaluate the skin condition surrounding the insertion site regularly, the tube’s location, and its integrity. Feeding, medication, and cleansing procedures must be administered correctly and meticulously to guarantee patient safety and enough nourishment. Along with educating patients and careers on tube care, maintenance, and potential risks, continuous monitoring is also critical for symptoms of intolerance, aspiration, and tube-related issues.

Are feeding tubes dangerous?
As a result of tube feeding, there are a number of risks, such as infections and leaks around the tube. Some patients must also be physically restrained or given medication in order to prevent them from attempting to remove their feeding tubes. In rare cases, feeding tubes might result in fatalities or severe sickness.
Also Read : What are Common Foot Problems in Older Adults?
Does the tube size determine how well a person will receive nutrition?
The effectiveness of nutrition delivery is generally not directly correlated with feeding tube size; nutritional absorption and overall well-being are more greatly impacted by factors like the type of formula used, where the tube should be placed and maintained, and the person’s feeding tolerance.
Are there any alternatives to feeding tubes?
Indeed, there are other options to feeding tubes, such as oral intake when it’s practicable, altered food textures or consistencies, oral supplements, parenteral nutrition (intravenous feeding), and palliative care techniques that prioritise comfort and quality of life in situations when feeding tubes are not practical or preferred. These choices are made with each patient’s needs, treatment objectives, and health needs in mind.
Last words
Not only are there alternatives to feeding tubes, but also options that prioritize comfort and quality of life when feeding tubes are impractical or unwelcome. These include modified meal textures or consistencies, oral supplements, parenteral nutrition (intravenous feeding), and oral consumption if possible. Each patient’s demands, therapeutic goals, and health requirements are considered while making these decisions.
Also Read : Discuss How Seniors can Combat Health Problems they may Face?
